Epidemiology and Pathophysiology
Epidemiology
Diabetes is a major public health problem that is approaching epidemic proportions globally. Approximately 34.2 million Americans, or 10.5% of the US population, have diabetes, including 7.3 million Americans who have not been diagnosed yet.1

Source: CDC. Diabetes Info Cards. https://www.cdc.gov/diabetes/library/socialmedia/infocards.html.
Diabetes affects people of all races and ethnicities, but disparities exist.3
- American Indians/Alaskan Natives comprise the largest age-adjusted racial/ethnic group of people with diagnosed diabetes.
- The proportion of African American, Hispanic, and Asian American populations who have diabetes is higher than in the non-Hispanic white population.
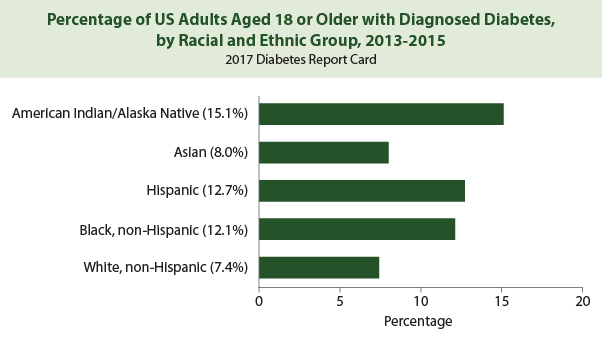
Source: CDC. Addressing Health Disparities in Diabetes. https://www.cdc.gov/diabetes/disparities.html.
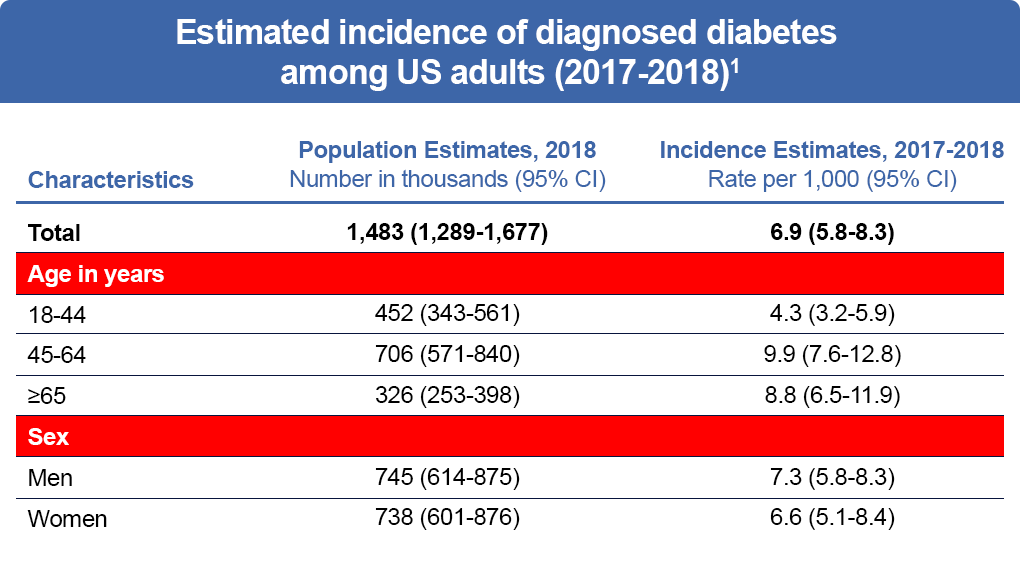
Approximately 1.5 million new cases of diabetes were diagnosed in adults in the United States in 2018. An estimated 452,000 new cases of diabetes occurred in patients age 18-44 years, 706,000 new cases in patients age 45-64 years, and 326,000 new cases in patients 65 years or older.1
Figure 3: Estimated incidence of diagnosed diabetes among US adults (2017-2018)1
In 2014 and 2015, approximately 5,700 people less than 20 years of age were diagnosed with type 2 diabetes each year.1
- The proportion of newly diagnosed cases in people under 20 years of age was higher among US minority populations than in non-Hispanic whites.1
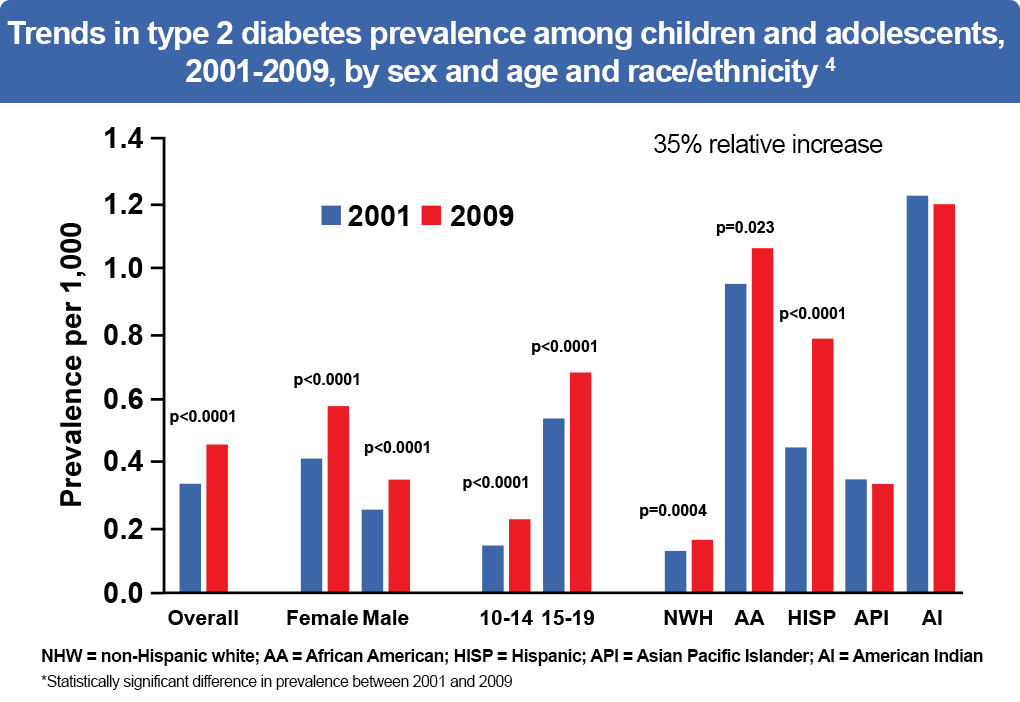
- Between 2001 and 2009, the adjusted overall prevalence of type 2 diabetes among children and adolescents increased by 30.5%.4
Figure 4: Trends in type 2 diabetes prevalence among children and adolescents, 2001-2009, by sex and age and race/ethnicity4
In 2018, 88 million Americans age 20 and older had prediabetes.1
- From 2013-2016, based on fasting glucose or A1c levels, 34.5% of US adults aged 18 years or older had prediabetes.1
- On the basis of fasting glucose or A1c levels, and after adjusting for population age differences, the percentage of US adults aged 20 years or older with prediabetes between 2013−2016 was similar for non-Hispanic whites (33.9%), non-Hispanic blacks (36.9%), non-Hispanic Asians (32.8%), and Hispanics (35.4%).1
Diabetes was the seventh leading cause of death in the United States in 2018.5
- The death rate from diabetes may be underreported.6
- Studies have reported that only about 35% to 40% of people with diabetes who died had diabetes listed anywhere on the death certificate.6
- Approximately 10% to 15% of death certificates had diabetes listed as the underlying cause of death.6
Pathophysiology
Diabetes is characterized by the dysfunction of insulin-producing pancreatic beta cells, insulin hormone resistance in cells of the body, or a combination of both.8,9
Figure 5: Pathophysiology of type 2 diabetes9
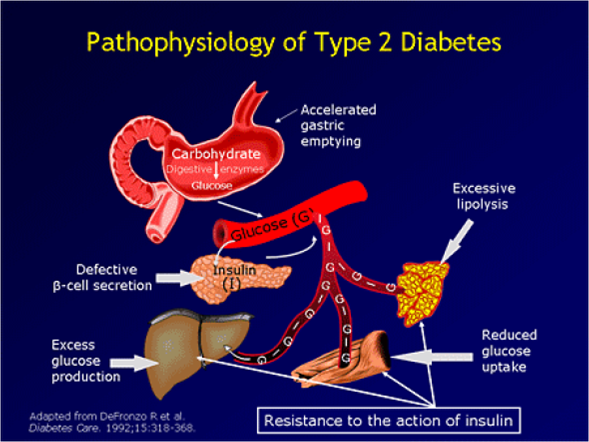
Five to ten years before most patients are diagnosed with diabetes, resistance develops to the effects of insulin in muscle and liver. Early on, in this state of “pre-diabetes,” pancreatic beta cells offset this resistance by increasing insulin secretion.10 Over time, insulin resistance in muscle worsens and pancreatic β-cells begin to fail, initially increasing post-prandial glucose levels. As insulin secretion declines further and the liver overproduces glucose at night, fasting plasma glucose levels subsequently rise.10,11 Progressive loss of β-cell mass and function continues as glucotoxicity worsens.10 Once insulin over-production no longer keeps pace with insulin resistance, plasma glucose levels remain persistently elevated.10 On average, patients have lost 50% to 80% of their β-cell function at diagnosis.11,12
Insulin resistance in muscle and liver and progressive pancreatic β-cell dysfunction represent only three of at least eight core defects implicated in the pathogenesis of type 2 diabetes.11
- Insulin resistance in fat cells increases the release of free fatty acids from triglycerides and further contributes to pancreatic β-cell death.11
- In response to food, the gut releases two incretin hormones, GLP-1 and GIP. Incretin hormones bind to pancreatic cells, increasing insulin production from β-cells and decreasing glucagon release from α-cells. In type 2 diabetes, incretin production is significantly reduced and β-cells become resistant to incretin effects, reducing insulin secretion.13,14
- Hepatic glucose production is further exacerbated by the overproduction of glucagon from pancreatic α-cells in both fasting and post-prandial states.11 As plasma glucose levels rise, excess plasma glucose is reabsorbed by the kidneys, instead of being excreted, contributing to hyperglycemia.11,15
- CNS resistance to the effects of insulin contributes to decreased satiety, weight gain, and peripheral insulin resistance in muscle and liver.11
References
- Centers for Disease Control and Prevention (CDC). National Diabetes Statistics Report, 2020. Atlanta, GA: Centers for Disease Control and Prevention, US Department of Health and Human Services; 2020. https://www.cdc.gov/diabetes/data/statistics/statistics-report.html.
- CDC. Diabetes Info Cards. https://www.cdc.gov/diabetes/library/socialmedia/infocards.html.
- CDC. Addressing Health Disparities in Diabetes. https://www.cdc.gov/diabetes/disparities.html.
- Dabelea D, et al. SEARCH for Diabetes in Youth Study. Prevalence of type 1 and type 2 diabetes among children and adolescents from 2001 to 2009. JAMA. 2014;311:1778-1786.
- Xu JQ, Murphy SL, Kochanek KD, Arias E. Mortality in the United States, 2018. NCHS Data Brief, 355. Hyattsville, MD: National Center for Health Statistics. 2020. https://www.cdc.gov/nchs/products/databriefs/db355.htm#section_2.
- American Diabetes Association. Statistics about diabetes. https://www.diabetes.org/resources/statistics/statistics-about-diabetes?loc=db-slabnav.
- Levin PA. Practical combination therapy based on pathophysiology of type 2 diabetes. Diabetes Metab Syndr Obes. 2016;9:355-369.
- Kahn SE, et al. Pathophysiology and treatment of type 2 diabetes: perspectives on the past, present, and future. Lancet. 2014;383:1068-1083.
- DeFronzo RA, et al. Pathogenesis of NIDDM. A balanced overview. Diabetes Care. 1992;15:318-368.
- Weir GC, Bonner-Weir S. Islet β cell mass in diabetes and how it relates to function, birth, and death. Ann N Y Acad Sci. 2013;1281:92-105.
- DeFronzo RA, Eldor R, Abdul-Ghani M. Pathophysiologic approach to therapy in patients with newly diagnosed type 2 diabetes. Diabetes Care. 2013;36(suppl 2):S127-S138.
- Butler AE, Janson J, Bonner-Weir S, et al. β-cell deficit and increased β-cell apoptosis in humans with type 2 diabetes. Diabetes. 2003;52:102-110.
- Drucker DJ. Enhancing incretin action for the treatment of type 2 diabetes. Diabetes Care. 2003;26:2929-2940.
- Meloni AR, DeYoung MB, Lowe C, et al. GLP-1 receptor activated insulin secretion from pancreatic β-cells: Mechanism and glucose dependence. Diabetes Obes Metab. 2013;15:15-27.
- Gerich JE. Role of the kidney in normal glucose homeostasis and in the hyperglycaemia of diabetes mellitus: Therapeutic implications. Diabet Med. 2010;27(2):136-142.








